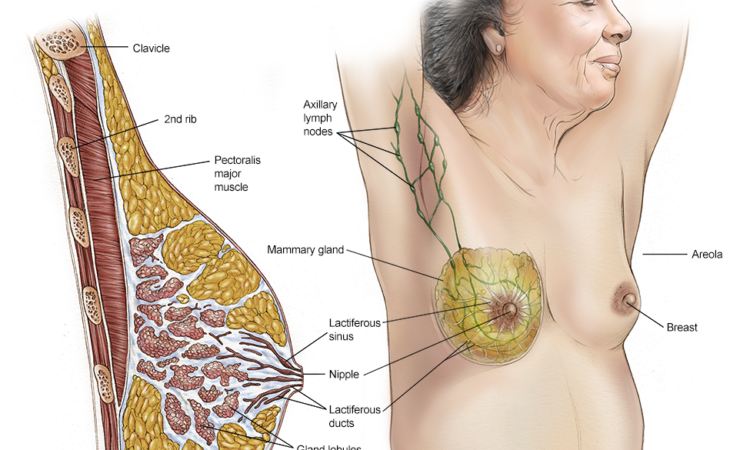
Endometriosis is a disease of the sexual organs of a woman characterized by the presence of cells in the lining of the womb (endometrium) outside the womb (ectopic cells). These cells (and their stroma) resemble cells inside the cavity (endometrium) and exhibit secretory activity. They respond to hormonal changes in the menstrual cycle, resulting in a chronic inflammatory response. This process results in internal bleeding, the development of painful nodules, inflammation, scarring, adhesions, and changes in the anatomical relationships of the organs in the smaller pelvis.
The disease is one of the most common causes of hospitalization in gynecological departments and the second, after myomas, a cause of hysterectomy (removal of the uterus).
Endometriosis is a “mystery” disease, and its cause has not been fully established.The etiological factors include congenital, environmental, epigenetic, autoimmune, and allergic factors. It is believed that the primary mechanism for the formation of endometriotic foci is retrograde menstruation, i.e., the passage of menstrual blood through the fallopian tubes into the peritoneal cavity and the implantation of exfoliated endometrial cells. However, since this mechanism is also observed in healthy women, other factors must also contribute to the formation of endometriosis foci.
In many women, endometriosis causesinfertility, chronic pain and thus worsening of the quality of life. It also represents a significant financial burden on health systems, for example in Austria the total annual cost of treating women for endometriosis is EUR 300 million and is comparable to the cost of caring forParkinson’s patients.
In this article, Niketrainers.com.co will tell you:
How common is endometriosis?
It is estimated that the disease occurs in 6-10% of all women of reproductive age, but it is most often diagnosed during diagnostic laparoscopic interventions in women with chronic pelvic pain syndrome (50-80%) and in infertile women (35-50%). ). It is estimated that nearly 180 million women are sick worldwide. There is no justification for the belief that the incidence of endometriosis is increasing, although better and better methods of diagnosis may lead to greater detection of the disease.
The risk factors for the development of endometriosis include: family conditions (3–10 times higher probability in women whose first-degree relatives suffer from endometriosis), impaired outflow of menstrual blood from the uterus to the outside (uterine malformations, previous infections, injuries and surgical interventions) ), early onset of the first menstruation (menarche) and short (<27 days) menstrual cycles and childlessness.
How is endometriosis manifested?
The most common symptom of endometriosis is pain in the small pelvis. Women may complain of dysmenorrhea, dyspareunia (painful intercourse), pain while urinating and passing stools, abdominal and back pain, and chronic pelvic pain (i.e. chronic abdominal pain lasting at least 6 months regardless of the phase of the menstrual cycle). Cyclicalsciaticapainin the lower limb and cyclical bleeding from the rectum or genital tract are less common. In very rare cases of lung endometriosis, it may experience periodichaemoptysisorshortnessof breath .
In women with endometriosis, symptoms from the lower gastrointestinal tract, such asflatulence,diarrhea, diarrhea alternating withconstipation, and urinary tract symptoms, such as urgency orpollakiuria, may also occur .
The disease is often asymptomatic and is diagnosed by chance, e.g. during various surgical interventions or during gynecological follow-up (e.g. endometriosis foci in the vagina or cesarean scar). Sometimes the only symptom is reduced female fertility. The severity of pain does not always reflect the severity of your endometriosis.
The appearance of dysmenorrhea in a woman who has not yet complained about this ailment, seriously suggests the suspicion of endometriosis. In such cases, diagnostic procedures should be started immediately (especially in young women), as it has been noticed that there is often a significant delay (even by 7–12 years) in the final diagnosis of the disease. Almost 75% of teenagers with pelvic pain are later diagnosed with endometriosis.Endometriosis should always be suspected if there is pelvic pain that is not primary menstrual pain.
How is the diagnosis of endometriosis made by the doctor?
Endometriosis is diagnosed on the basis of clinical symptoms, gynecological palpation, imaging tests (most often ultrasound examination [USG], sometimesmagnetic resonance imaging(MRI)) and the image found during the surgical intervention (laparoscopy), confirmed by histological examination of the samples taken .
Gynecological examination of endometriosis
During the gynecological examination, the doctor assesses mainly the position, size, and mobility of the uterus and appendages (ovaries and fallopian tubes), sacro-uterine ligaments (ligaments connecting the back wall of the cervix with the rectum and sacrum—a frequent location of endometriosis) and the rectovaginal septum (connection between the walls of the vagina and rectum).
The last two items are best assessed by a simultaneous vaginal-rectal examination (the doctor inserts the index finger into the vagina and the middle finger into the rectum). Performing the test during menstruation increases the chance of detecting foci of deeply infiltrating endometriosis!
Imaging studies
The basic diagnostic examination is both vaginal and rectal ultrasound. The ultrasound image of endometrial cysts (cysts located in the ovary) is quite characteristic. These cysts have thick and fibrotic walls and are filled with dense content (hemolyzed blood). In the diagnosis of deeply infiltrating endometriosis, ultrasound performed through the rectum is used, especially in women reporting intestinal complaints (intestinal dysfunction and episodes of rectal bleeding during menstruation) and in the case of suspicion of changes in the colon wall and a focal lesion in the posterior region vaginal forks (diameter ≥3 cm). MRI (with a full bladder) is also a useful test.
Laparoscopy
Laparoscopy is now considered the “gold standard” in the diagnosis of endometriosis. According to the recommendations of the Polish Gynecological Society of 2012, laparoscopy should be performed especially in women:
- suffering from dyspareunia, dysmenorrhea and chronic pain, in whom the quality of life is deteriorating and pharmacological treatment is ineffective or contraindicated,
- in whom, during a gynecological examination, the presence of painful nodules in the sacro-uterine ligaments,
- who have been diagnosed with nodular changes in the appendages, and
- infertile in whom diagnostic tests show no abnormalities.
It is recommended to perform a histological examination of all the collected or removed tissues in order to make a simultaneous diagnosis.
Other diagnostic tests for endometriosis
In justified cases where deeply infiltrating endometriosis is suspected, especially in the area of the bladder and large intestine, cystoscopy and/or orcolonoscopycan be performed.
There is no clear evidence to support the routine determination of the tumor marker CA-125 (cancer antigen 125). It is known that its concentration is increased in cases of moderate and severe endometriosis, but its sensitivity (i.e. the probability of detecting the disease) does not exceed 30%. On the other hand, in justified cases, the determination of the concentration of CA-125 sometimes helps in making decisions about the further procedure.
What are the treatments for endometriosis?
Treatment of endometriosis, due to the high rate of disease recurrence, is a hot topic of discussion in the medical community. Pharmacological, surgical and combined methods (both methods) are used. The choice of the treatment method depends on its clinical effectiveness, tolerance and costs of therapy, the doctor’s experience and the degree of patient cooperation. An important factor determining the choice of the method are the maternal plans of the treated woman.
Pharmacotherapy
The principle of treatment is to induce amenorrhea and create a state of hypoestrogenism, which theoretically should prevent the growth of the endometrium and promote the regression of lesions and pain relief. However, symptoms of the disease may reappear after discontinuation of therapy.
Pharmacotherapy includes: hormonal contraceptives (estrogen-progestins),gonadotropin-releasing hormone agonists(Gn-RH) analogues, progestins, less frequently danazol and aromatase inhibitors (most often together with DTA). All drugs show similar effectiveness in reducing the intensity of pain associated with endometriosis and the duration of improvement after the end of treatment.
Oral contraceptive pills (DTAs)have been used empirically for many years in the case of dysmenorrhea and are considered by SA as the method of choice to start therapy when endometriosis is suspected. DTA is used both cyclically (inducing menstruation every 28 days) and continuously (without inducing menstruation). The latter method is usually used in women in whom the cyclic method did not bring a satisfactory effect. DTA is as effective as Gn-RH analogues in treating pain associated with endometriosis, but does not induce hypoestrogenism (risk of bone mineral density reduction –osteoporosis) and can be used for a long time. The risk of side effects is the same as when using hormonal contraception.
Progestogensinhibit the growth of endometriotic implants, leading to their atrophy (disappearance). Progestogens can be administered orally, intramuscularly, or in the form of hormone-releasing intrauterine systems. The latter method is particularly applicable to women with heavy menstruation caused by the presence of endometriotic foci in the uterine muscle (adenomyosis). It has also been shown that the progestin-releasing system reduces pain in women who have undergone surgery for endometriosis. Side effects of progestogens include weight gain, fluid retention, depressed mood, and acyclic bleeding.
Danazolinhibits the synthesis and release of gonadotropins and the synthesis of ovarian hormones.
The effectiveness in combating pain is comparable to that of other drugs, but due to the androgenic effects and the associated undesirable effects, incl. oily skin,acne, weight gain and hirsutism are rarely used today. Danazol can also cause emotional lability, hot flushes, vaginal dryness and a temporary reduction in the volume of the breasts (hypoestrogenism). The drug is usually used at a dose of 600–800 mg per day, although it has been shown to be effective also with lower doses.
Gonadoliberin analoguesthat reduce pituitary gonadotropin secretion have been used until recently as first-line pain therapy in moderate to severe endometriosis. The drug is administered intramuscularly, subcutaneously or intranasally. When fighting pain, this group of drugs does not improve fertility rates in a woman. Due to the undesirable effects associated with hypoestrogenism (including the risk of developing osteoporosis), add-back therapy is oftenusedwithagonists. Therapy usually lasts up to 6 months. The price of drugs is a significant limitation.
Non-steroidal anti-inflammatory drugs (NSAIDs)are used in the treatment of pain associated with endometriosis . Although their effectiveness has been shown mainly in women with primary dysmenorrhea (not related to endometriosis), these drugs are commonly used in the treatment of endometriosis, mainly because of relatively low side effects, moderate cost and high availability.
The effectivenessof aromatase inhibitors(an enzyme that plays a key role in the process of steroidogenesis – the production of estrogens and gestagens) in the treatment of endometriosis has been demonstrated in several clinical studies. This drug was given with a progestin or DTA due to the significant risk of overstimulation of the ovaries and cyst formation. No reduction in bone mineral density was observed during the 6-month treatment.
None of the presented methods of pharmacotherapy lead to complete cure and have no beneficial effect on pregnancy. Therefore, the initiation of hormone therapy in women who are unable to become pregnant with diagnosed (suspected) endometriosis is delaying, sometimes for many months, basic (surgical) treatment, as appropriate drugs induce pharmacological infertility.
Surgical treatment
The indications for surgical treatment of endometriosis include pelvic pain, infertility in the course of endometriosis, deeply infiltrating endometriosis, and ovarian endometrial cysts (> 3 cm in diameter).
Conservative surgical treatment
bladder and blood vessels (uterine arteries) or near these organs. Therefore, these interventions should be carried out in specialized centers by experienced doctors. Inadequate resection of endometriotic lesions is a common cause of persistent symptoms or relapses. Conservative surgery benefits infertile women with mild to moderate disease severity and removal of cysts> 3 cm in diameter. However, it has not been unequivocally established whether removal of foci of deeply penetrating endometriosis improves fertility rates, although in some studies the effectiveness of such a procedure was observed even 50%. Inadequate resection of endometriotic lesions is a common cause of persistent symptoms or relapses. Conservative surgery benefits infertile women with mild to moderate disease severity and removal of cysts> 3 cm in diameter. However, it has not been unequivocally established whether removal of foci of deeply penetrating endometriosis improves fertility rates, although in some studies the effectiveness of such a procedure was observed even 50%. Inadequate resection of endometriotic lesions is a common cause of persistent symptoms or relapses. Conservative surgery benefits infertile women with mild to moderate disease severity and removal of cysts> 3 cm in diameter. However, it has not been unequivocally established whether removal of foci of deeply penetrating endometriosis improves fertility rates, although in some studies the effectiveness of such a procedure was observed even 50%.
The method of choice is laparoscopy, an intervention that is relatively safe and well tolerated by patients. Laparoscopy (compared to laparotomy) is associated with a shorter hospital stay, a lower complication rate and a lower postoperative morbidity. However, it should be remembered that there are, but rarely, serious complications, including damage to the intestines, bladder, ureters, and large vessels.
Radical surgical treatment
In particularly severe cases (lack of effectiveness of pharmacotherapy and conservative surgical treatment) and in women not planning pregnancy, radical surgical treatment is used – removal of the uterus and ovaries. Its purpose is to induce surgical menopause. However, this intervention does not completely cure all the operated women, and pain symptoms still occur in 15% of them. The preservation of the ovaries is associated with a several times greater risk of the need for another surgical intervention than in the case of their removal. Removal of the uterus with (or without) appendages in women with deep endometriosis may be associated with similar difficulties as resection of endometriotic implants only. The operation should be performed by an experienced physician in a specialized center.
What is the next procedure?
The way to proceed is individual. In women who do not plan to become pregnant, the primary goal is to return to normal daily activities and work, which is primarily associated with pain control. Since relapses occur quite frequently, pharmacological treatment courses are repeated, taking into account the effectiveness of previously used methods and the patient’s preferences, although DTA and NSAIDs are the most commonly used. There is rarely a need for a second operative intervention.
Women planning motherhood should try to get pregnant immediately after the end of surgical treatment. The lack of results is an indication, according to many experts, for in vitro fertilization, and not for another surgical intervention.
Data on the influence of endometriosis on the course of pregnancy are ambiguous. Contrary to popular belief, pregnancy does not “cure” endometriosis, but only temporarily inhibits the development of the disease. There have also been reports of intraperitoneal bleeding in pregnant women with endometriosis.
Summary
Endometriosis, although often asymptomatic and is diagnosed accidentally during a control gynecological examination, may be a chronic disease that is difficult to cure, and in severe forms may impair a woman’s daily and professional activity. It is also a common cause of infertility. The disease affects all women of childbearing age, including young and very young women. The leading symptom of endometriosis is pelvic pain, especially painful periods (acyclic pain is more common in young women). In such cases, the diagnosis of pain should include endometriosis. A delay in diagnosis and treatment implementation may result in the development of the disease, worsening of changes in the pelvic organs, and infertility.
In women who are diagnosed with endometriosis (or are suspected of having the disease) planning to become pregnant, surgical treatment is not recommended.