Polymyalgia Rheumatica is an inflammatory disease from the group of the so-called systemic connective tissue diseases, manifested mainly by pain and stiffness in the muscles of the neck, shoulder and hip girdles. It is the most common disease in this group of elderly people. Sometimes it develops slowly over a period of months, and sometimes the symptoms increase rapidly.
In this article, Niketrainers.com.co will tell you:
Factors contributing to the occurrence
It is not known why polymyalgia mainly affects the elderly (it is practically not found before the age of 50). Its incidence increases with age. A genetic predisposition to polymyalgia has been demonstrated. Other factors that are likely to contribute to the development of the disease include solar radiation and viral infections. The mechanism of action of these factors is not fully understood.
How common is polymyalgia?
It typically occurs after the age of 50. Women are sick twice as often as men. It is also more common in white people. It is geographically diverse – most cases are recorded in Northern Europe, while in southern Europe it is almost unknown.
How is polymyalgia manifested?
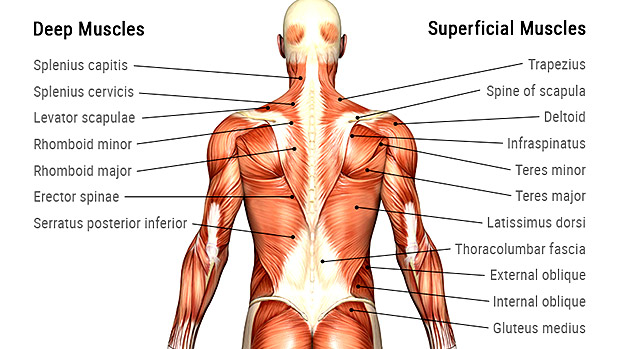
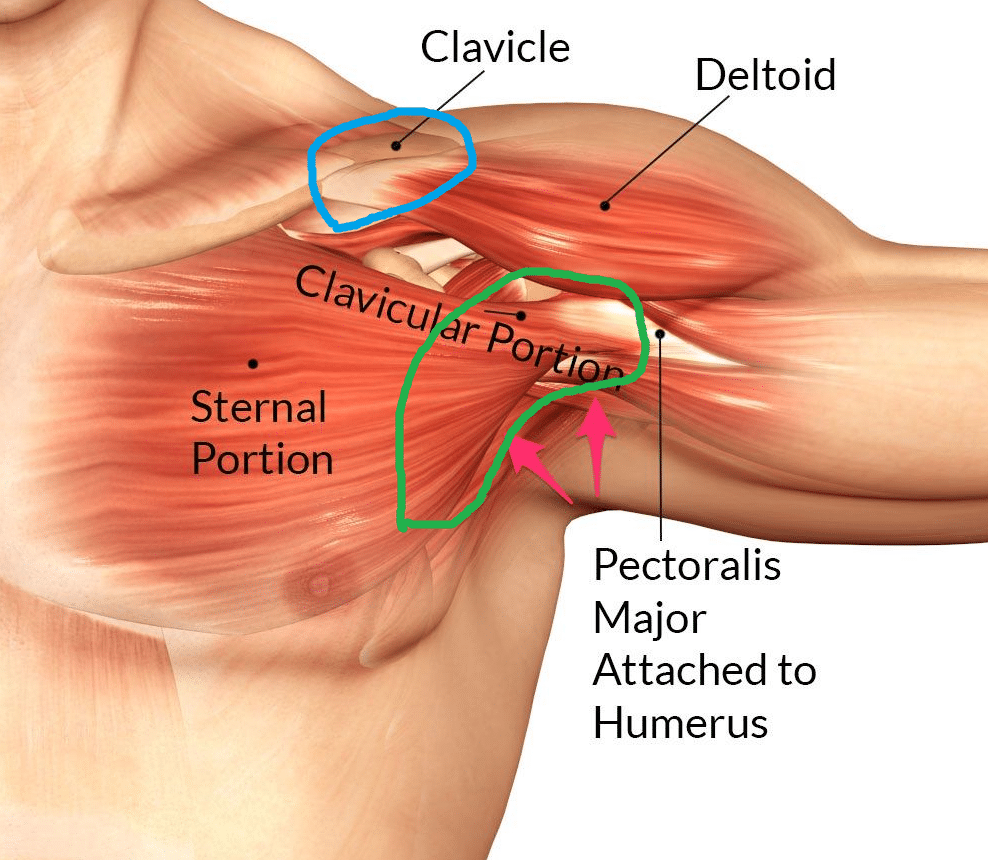
Polyymalgia is characterized by pain in the muscles of the shoulder girdle, hip girdle, and the neck and nape. Muscles are painful to pressure, but their strength is normal. Muscle weakness and atrophy may occur in advanced disease, secondarily. Accompanying symptoms are:
- morning stiffness of painful muscle groups (lasting more than 30 minutes)
- arthritis (most often knee and sternoclavicular joints)
- pastyswellingof the distal parts of the limbs (hands and feet)
- low-grade fever andfever
- general feeling of being unwell.
Patients also complain of low mood, sleep disorders anddepression.
What to do in the event of symptoms?
You should see your GP.
In the case of multiple symptoms, not only for muscles, patients quickly seek medical help. When the disease progresses slowly or affects one muscle group, the symptoms are often attributed to other diseases common to the elderly. Very often, the reason for initiating intensive diagnostics is the presence of a significantly accelerated ESR (sometimes over 100 after the first hour).
How is the diagnosis made by the doctor?
The diagnosis is usually made by a rheumatologist, mainly on the basis of symptoms reported by the patient and the results of basic blood tests.
Among the clinical symptoms, the most important thing is the presence of pain in at least 2 out of 3 muscle groups:
- shoulder girdle
- hip girdle
- neck / nape.
An additional symptom concerning muscles is the feeling of their stiffness after immobilization (after a night of rest or prolonged immobility), lasting at least 1 hour.
Laboratory tests show:
- accelerated ESR (often> 100 ml / h), but normal ESR does not exclude the disease
- high concentration of CRP (C-reactive protein) andfibrinogen
- increase in alkaline phosphatase.
In the case of arthritis or tendon sheath inflammation, imaging tests, such as ultrasound of the musculoskeletal system and MRI, are helpful in assessing the severity of inflammation.
The age of the patient is not without significance for the probability of diagnosis. Diagnostics should be performed to exclude neoplastic disease, because in the case of manyneoplasms, the first symptoms resemble those occurring in the course of rheumatic polymyalgia.
In order to establish a certain diagnosis, criteria developed by a team of scientists are used, most often the diagnostic criteria according to Bird and Woodd and the Healer criteria.
What are the treatments?
The most important drugs used from the moment of diagnosis of the disease are glucocorticosteroids –prednisoneand its derivatives. Significant improvement after the use of prednisone 72 hours after the start of treatment confirms the accuracy of the diagnosis.
The drug is administered orally in a single dose in the morning after a meal. After using this dose for about a month, attempts are made to reduce it.
Glucocorticosteroids are very effective drugs and they are used of choice in polymyalgia, but due to numerous side effects they should be administered in the lowest effective dose and for the shortest possible time.
Rheumatic polyymalgia very often requires long-term treatment with glucocorticosteroids (up to several years, at least 1-2 years).
Dosage reduction of the glucocorticoid often leads to a recurrence of symptoms. Then attempts are made to add another drug from the group of immunosuppressants –methotrexate.
Non-steroidal anti-inflammatory drugs are useful for maintenance therapy.
In the case of steroid therapy lasting more than 3 months, the prophylaxis ofosteoporosisin the form of vitamin D and calcium supplements should be additionally implemented, and the administration of a bisphosphonate anti-osteoporosis drug should be considered.
After acute inflammation is under control, rehabilitation is recommended, aimed at maintaining muscle strength, preventing joint contractures and preventing falls.
Is it possible to recover completely?
Rheumatic polyalgia is a curable disease. Most patients benefit from steroid therapy. The prognosis is good.
Sometimes there is a tendency to spontaneous extinction of the disease.
Relapses most often occur in the first two years of the disease. The disease rarely lasts more than 5 years.
What do I have to do after treatment is finished?
Long-term follow-up is required after the end of treatment. Muscle pain and other accompanying symptoms are monitored, and laboratory tests mainly show ESR. During treatment and after its completion, observation of possible complications of steroid therapy is required.
What to do to avoid getting sick?
The disease is immune in nature; its cause is unknown. Genetic factors beyond our control are taken into account.It is also suspected that viruses and bacteria (parvovirus B19, Mycoplasma pneumoniaeandChlamydia pneumoniae), solar radiation and smoking (in women) are involved in the development of the disease .
There are no known methods of preventing the disease. It is recommended to lead a hygienic lifestyle.
Attention
About 20% of people with rheumatic polymyalgia also have
giant cell arteritis, and 40–60% of people with giant cell arteritis show symptoms of rheumatic polymalgia.Giant cell arteritis with the involvement of the head arteries, which may lead to blindness, is an absolute indication for urgent treatment.