A bedsore is a pressure ulcer that develops in long-term lying people as a result of chronic pressure or rubbing of the skin.Treatment of pressure ulcers is difficult, so prevention of bedsores is very important. Proper hygiene and care of the sick person, as well as the use of anti-bedsore mattresses, play an important role in preventing the formation of pressure ulcers.
In this article, Niketrainers.com.co will tell you:
What are pressure ulcers and what are their causes?
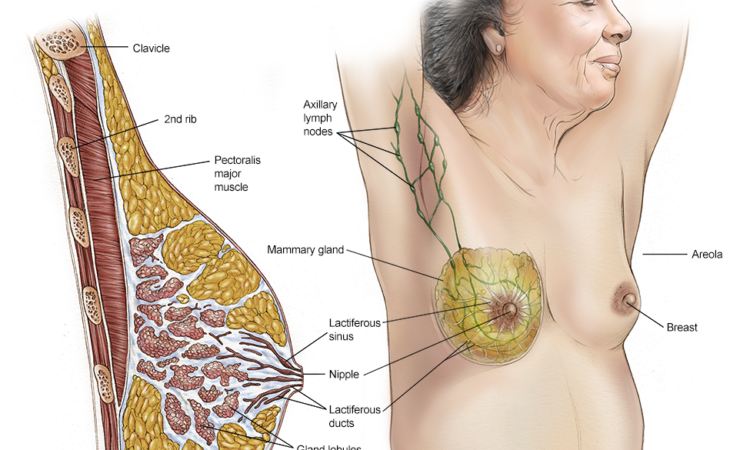
A pressure ulcer is a pressure ulcer that develops in long-term lying people as a result of chronic pressure or rubbing of the skin. The most common places of occurrence are the sacrum, buttocks or heels in immobilized patients (patients with paralysis, sensory disturbances, after injuries). Other common areas where pressure ulcers occur are the elbows, knees, and ankles. Pressure ulcers can also develop under a plaster cast. Especially in children, their development can occur very quickly, within a few days of putting on the plaster cast. The essence of the disease process in the case of pressure ulcers is ischemic necrosis of the skin and sometimes of deeper tissues.
The risk of developing pressure ulcers increases in patients who are improperly cared for, suffer from impaired sensation and mobility, low blood pressure,urinaryand stool incontinence, as well as infracturesand nutritional disorders.
How common is pressure ulcer?
Pressure ulcers are particularly common in patients staying at home or in a care and treatment facility – in 7–23%, in neurological wards – in 12%, in rehabilitation wards – in 6% and in 14–25% of patients with advanced neoplastic disease.
Classification of pressure ulcers
Bedsores, depending on the advancement of the lesions, can be divided into degrees. The higher the grade, the greater the tissue damage and the more difficult the treatment.
Clinical classification of pressure ulcers (according to Torrance):
- Grade I:fading redness– reactive hyperemia and redness in response to injury. After pressing with a finger, the skin turns pale, which means that the microcirculation is still undamaged.
- stage II: non-blushing redness– erythema that persists after the pressure has ceased indicates microcirculation damage, inflammation andswellingof the tissues. The following may appear: superficial swelling, epidermal damage and blisters.
- stage III:ulceration– damage to the full thickness of the skin (epidermis and dermis) to the border with the subcutaneous tissue. The edges ofthe woundare surrounded by swelling and erythema. The bottom of the wound is filled with red granulation tissue (the tissue formed during wound healing) or yellow masses of disintegrating tissue.
- stage IV:damage also extends to the subcutaneous tissue to the boundary with the fascia. Fat necrosis is caused by inflammation and thrombosis of the small blood vessels. The edge of the pressure ulcer is usually well-defined, but necrosis can also involve surrounding tissue. The bottom may be covered with brown-black necrosis.
- Grade V:advanced necrosis extends beyond the fascia and affects muscles, and sometimes also tendons, joints and bones. There are cavities that can be connected to each other. The wound contains disintegrating masses of tissues and black-brown necrosis.
Pressure ulcers, like other wounds, can become secondary bacterial infections and then become covered with a green-yellow purulent discharge, accompanied by redness around the wound and sometimes a foul odor.
Symptoms of pressure ulcers
The finding of pressureless erythema in pressure areas in a lying / immobilized patient is an indication for prophylaxis, including changing the patient’s position (every 2 hours or even more often) and massage of these areas when changing position, as well as the use of anti-bedsore mattresses, which consist of separate sections are alternately automatically filled with air, so that the constant pressure on the skin of the patient lying down is replaced by alternating pressure. Anti-bedsore mattresses and pillows are co-financed by the National Health Fund for bedridden patients eligible for such prophylaxis (www.pfron.org.pl). In the event of the development of an ulcer, medical consultation and appropriate treatment are recommended. Appearance of soreness around the wound withfever and chills may indicate panniculitis and is an indication for urgent consultation.
What to do in the event of pressure ulcer symptoms?
The diagnosis of pressure ulcer is based on a medical examination. Usually a clinical picture is sufficient. If a bacterial superinfection is suspected, a swab from the wound is taken. Complications such as osteomyelitis may require additional investigations.
Treatment of pressure ulcers
Treatment of pressure ulcers is often difficult and long-lasting, therefore the doctor’s instructions regarding the care and hygiene of the pressure ulcer and its vicinity should be meticulously followed. Currently, there are many ready-made dressings for the treatment of pressure ulcers, each material has its own specificity and specific action, which makes it effective in the treatment of pressure ulcers of a specific stage.
Treatment of pressure ulcers depends on their severity.
- Stage I– it is necessary to urgently relieve the pressure from the area, apply proper skin hygiene and observe. Polyurethane membranes are used – thin, flexible, transparent dressings that protect the skin exposed to pressure by reducing the friction force. The inner side of the membrane adheres to the skin. The structure of the membrane allows for evaporation from the surface of the skin, but it is impermeable to water and pollutants from the outside. It can stay in place for up to 10 days.
- Stage II– apart from the immediate relief of the damage site, the pressure ulcers are covered with a super-thin hydrocolloid dressing, which absorbs the secretions, may remain on the bedsores for a long time and creates a moist environment favorable for the healing processes.
- Stage III– pressure ulcer usually requires removal of necrosis. If there is no clear separation from healthy tissues, initially hydrocolloids or hydrogels are used, and then surgical debridement is performed.
- Stage IV and Vpressure ulcers are treated surgically. Conservative (non-surgical) treatment is carried out if the patient does not qualify for surgery, and as a preparation for surgery – until the bottom of the ulcer is covered with granulation tissue (tissue formed during healing).
It is possible to heal the pressure ulcer, especially in stage I and II, if the pressure is relieved. A particularly dangerous complication of bedsores, especially grade III and IV, is osteomyelitis, which is associated with the development of sepsis and high mortality.
In the case of healed bedsores, it is advisable to implement prophylactic and therapeutic elements to prevent the occurrence of further ulcers. The use of appropriate anti-bedsore mattresses, frequent change of body position, appropriate skin care, and above all, treatment of causal diseases and quick mobilization of patients are an important element preventing the development of pressure ulcers.
Pressure ulcer prevention
Prevention is a series of activities, treatments and the use of equipment to reduce the impact of harmful factors and the risk of pressure ulcers. After a wound has formed, continued prophylaxis is essential to improving healing conditions.
The general procedureincludes:
- care for the general condition and nutritional status of the patient,
- education and, if possible, increasing the patient’s activity,
- in completely dependent patients – regular change of position, stabilization of the patient’s position using appropriate supports and rollers, ensuring air access to the skin, protection against urinary and stool incontinence,
- use of delicate cotton bed linen and personal linen.
Polyurethane dressings can be used on places particularly exposed to pressure.
It is very important to use anti-bedsore mattresses and pillows. Particularly useful are dynamic pressure swing mattresses, the operation of which consists in the fact that separate chambers of the mattress are alternately filled with air from the compressor. This causes a cyclical reduction in pressure, which improves the blood supply to the skin areas not currently in contact with the mattress. Variable pressure mattresses with time-adjustable slight (up to 20 °) lateral tilt or adjustable one- or two-sided patient rotation up to 30 ° are gaining popularity.
In anti-bedsore cushions, pressure changes are achieved with a compressor or a hand pump, and may be equipped with a shape memory function.








































![The funeral procession for Murphy Afolabi ended at his home in Ikorodu [VIDEO].](https://niketrainers.com.co/wp-content/uploads/2023/05/Brown-Elegant-Fashion-Sale-Website-YouTube-Thumbnail-34-750x450.png)
![[VIDEO] Kolawole Ajeyemi weeps terribly over the loss of Murphy Afolabi.](https://niketrainers.com.co/wp-content/uploads/2023/05/Brown-Elegant-Fashion-Sale-Website-YouTube-Thumbnail-33-750x450.png)